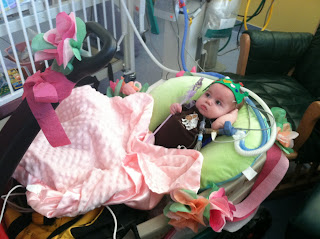
Norah had yet another trip to the OR on Monday. Many (if not most) special-needs moms could tell you exactly how many times their child has gone to surgery. I lost count long ago. This time she went in for her trach scar revision, and it'll be great to see how everything heals. I hope she grows to be proud of her scar and what she's overcome. Our ENT also noted that her mid-airway still has quite a bit of tracheomalacia (her airway doesn't stay rigid & open - think of a straw that is pinched half-way closed). He knows that I love pictures so brought some out to me. Hopefully she grows out of that floppy airway. This particular trip to the OR was particularly stressful because it was her first since having her trach out. But everything went smoothly without any issue. We walked away feeling relieved that Norah wouldn't need surgery for a LONG time.
We were wrong.
We went to Shriner's to follow-up with her Orthopedic doctor. We've known that Norah's neck isn't totally stable (she has excessive movement between C1 & C2) but we've hoped that over time, things would ossify and strengthen & she'd be fine. Turns out, it's gotten worse. We have a bunch of appointments next week, but I'm under the assumption that they're going to want to fuse Norah's neck within the next couple weeks.
I know that fusion will help her be stable, safe, and prevent spinal cord injury. But I am scared. I am scared of pain and her own fear. I am scared she won't want to come off the ventilator post-op. I am scared of permanent injury. I am scared of death. Of course, not getting this surgery could lead to those same things. So I know it is necessary. But that doesn't make it easier.
The thing is: I know Norah can do this. She has been through so much and has shown us that she isn't going to give up. I mostly worry about my own ability to hold it together. I hate seeing her hurt. I hate that I can do so little to protect her from the inevitable pain associated with her medical woes. I hate that our family will again have to taste what it is like to be apart. I hate that Harper has to see his mom cry this way. I hate that he has such worry about Norah in the hospital. He said to me recently, "But mom, I thought we got to keep her. I don't want her to go to the hospital."
So again we go through another challenge together. Part of me has forgotten that life in the hospital. I don't know how we endured those 23 consecutive months. But then the other part of me remembers that time with such distinct clarity that it adds to the anxiety and fear of going through that again.
I'll try to keep you all updated on her upcoming schedule. Here's to strength, bravery, and love getting us through.
We were wrong.
We went to Shriner's to follow-up with her Orthopedic doctor. We've known that Norah's neck isn't totally stable (she has excessive movement between C1 & C2) but we've hoped that over time, things would ossify and strengthen & she'd be fine. Turns out, it's gotten worse. We have a bunch of appointments next week, but I'm under the assumption that they're going to want to fuse Norah's neck within the next couple weeks.
I know that fusion will help her be stable, safe, and prevent spinal cord injury. But I am scared. I am scared of pain and her own fear. I am scared she won't want to come off the ventilator post-op. I am scared of permanent injury. I am scared of death. Of course, not getting this surgery could lead to those same things. So I know it is necessary. But that doesn't make it easier.
The thing is: I know Norah can do this. She has been through so much and has shown us that she isn't going to give up. I mostly worry about my own ability to hold it together. I hate seeing her hurt. I hate that I can do so little to protect her from the inevitable pain associated with her medical woes. I hate that our family will again have to taste what it is like to be apart. I hate that Harper has to see his mom cry this way. I hate that he has such worry about Norah in the hospital. He said to me recently, "But mom, I thought we got to keep her. I don't want her to go to the hospital."
So again we go through another challenge together. Part of me has forgotten that life in the hospital. I don't know how we endured those 23 consecutive months. But then the other part of me remembers that time with such distinct clarity that it adds to the anxiety and fear of going through that again.
I'll try to keep you all updated on her upcoming schedule. Here's to strength, bravery, and love getting us through.



.JPG)
.JPG)